Her countenance exudes calm, but when her legs are crossed, her right foot probably is a better gauge of what is really going on with Valera Hudson, MD.
The foot, typically clad in a navy athletic shoe, is in constant motion.
She calls herself an “introvert by nature,” which she says is not to be confused with shyness, despite what the dictionary might say. Hudson favors author Susan Cain’s description: That introverts prefer quiet, minimally stimulating environs, quiet concentration, listening more than they talk and thinking well before they speak.
“Introvert just describes how you get your energy. It’s just what fills your tank, what charges your battery,” says Hudson.
A big thing charging Hudson’s battery is the wellbeing of children.
That is a good thing. Because it can be a tough world for children these days. Headlines highlight the latest school shootings. Assault is a leading cause of death in children ages 1 to 4, according to the Centers for Disease Control and Prevention. Suicide is a top killer among 10- to 14-year-olds. About 10% of children ages 3-17 have ADHD. An estimated one in six children in that age group have one or more developmental debilities that can impact every aspect of their being. It feels like a lot.
“I think collectively as a society we have a number of factors that have disrupted and changed the experience of children,” reflects Hudson, a 1985 Medical College of Georgia graduate who chairs her medical school’s Department of Pediatrics.
“I am not trying to make a value judgement, but things are different, meaning that many kids lives are chaotic and unpredictable. Our society runs 24-7. No one thinks they need any sleep, even though we are wired to need sleep just like we are wired to need food and water. There are families who are not even sure where their next meal is coming from and who are not safe in their own home,” she says.
Poverty and racism can make many matters worse. Too much money can create a different level of stress, like performance addiction and sometime unrealistic achievement expectations. Real connections with other people likely are not made through texting.
But there are also record numbers of premature babies, children with cancer, children born with heart defects and young victims of trauma surviving and thriving. The same day Hudson was talking a newborn, who was expected to die and who other hospitals had refused to take, went home with her parents from the Children’s Hospital of Georgia after just a few days on ECMO, which takes over the work of the heart and lungs, most often when a child is born in dire respiratory distress.
“We all live in paradox, the tension that two things that seem like they are opposite are true at the same time,” Hudson says. There may be no greater tension or paradox than the reality that while most children who get sick live, some will die. While death is heartbreaking, the risk is worth it, she says.
The MCG Department of Pediatrics and Children’s Hospital of Georgia exist to reduce the risk and soften the paradox.
“I can’t change how we got here,” Hudson says. “What I can address is how do we move forward. I can say we have some real challenges but part of being a pediatrician is that hope and expectation that we can intervene and make things better and that the hope of our country rests on our children.”
What children deserve
“Children deserve the care that we can provide here,” says the children’s hospital’s pediatrician-in-chief.
So, like the most intricate LEGO MOC (my own creation) ever made, Hudson has spent the last five years of her life ensuring that what the children get is great care.
That includes the basic of more physicians to take care of the diverse needs of children. This past year there’s been an unprecedented list of recruits to add depth and scope to what could be done specifically for children. It has meant new programs and tweaking others to better accommodate the state of children today. It has meant plans to grow the state’s second largest children’s hospital.
“We are growing broadly across the board in surgery and medicine,” Hudson says. Targeted clinical programs include strengthening the longstanding pediatric heart program, strengthening the pediatric cancer program with the addition of a bone marrow transplant program and a new emphasis on behavioral and mental health to better address that growing crisis in children.
The self-declared introvert did not pursue the job as boss of such important work, as much as it seemed to pursue her. She talks about standing on the shoulders of giants like Al Pruitt, MD, who chaired the department for a decade starting in 1982 and Bill Kanto, MD, a neonatologist and longtime division chief, who served as chair from 1994-2009. Both would become her mentors. She can still remember as an exasperated young faculty member saying to or at least around Kanto: You could not pay me enough to do your job. She wondered for a moment if she had actually said it aloud and knew that she had when he laughed. She would learn from these and others what good leadership is and from still others what it is not. “Everybody comes to things differently,” she says.
Pruitt, now an Episcopal priest, was chair while Hudson was still in medical school, and while she completed her pediatric residency at MCG and its health system, including a year as chief resident.
When she left for her three-year pediatric pulmonology fellowship in 1989, years she recalls as some of the best and hardest in her life, at the University of Minnesota Hospitals and Clinics in Minneapolis, she reasoned she was gone forever from the town where she was raised (but not born) by Don and Marie Hudson. But Pruitt, who she calls a servant leader, stayed in touch, reminding her what she could do for children back home. She would not have come back without him.
She returned as associate director of the Cystic Fibrosis Center and medical director of Pediatric Pulmonary Diagnostics. She became director of the Pediatric Residency Program in 1997 and kept it up for 20 years. She became vice chair of the Department of Pediatrics in 2008, chief of the Division of Pediatric Pulmonology in 2012 and six years later, first interim chair then chair of the Department of Pediatrics.
“If you have a chronic illness then you are more prone
to anxiety and depression. If you have anxiety and
depression you are more prone to not taking care of
yourself and doing your treatments and taking your
medicine. So, you can’t treat one and ignore the other
and expect to be successful.” – Valera Hudson, MD
Stepping up and out
Hudson had for years been stepping up to help her colleagues and her children’s hospital whenever she could, so it was logical to step up as again as interim. MCG Dean David Hess said then it was quickly clear when they started looking for a ‘permanent’ chair that the best person for the job was already in it.
Because Hudson never considered that ‘interim’ meant ‘temporary’ or worse ‘making do.’ “What I told folks from the beginning is if we do not have a thriving clinical service, we do not have a platform for teaching and for advancing the field through research,” says Hudson. As interim chair she was also interim pediatrician-in-chief of the Children’s Hospital of Georgia and her years of boots on the ground made her acutely aware of what was needed to shore up the three-legged academic stool.
Her department and the children’s hospital had lost too many faculty members in the most recent years, part of the reason there was no time to be reticent. She worked from day one as if she were already chair, knowing she would have to leave if that approach didn’t work and/or wasn’t appreciated. She was willing to take the risk because full tilt was all she knew and what she and longtime colleagues knew was needed. By then, she also wanted the job.
At the top of her list was distinguishing between the frontline work of the general pediatricians and the increasingly present pediatric hospitalists. Evolving trends in health care had drawn the distinction and broadened the divide between the skillsets of these two groups.
To shore up both, her first six interim months included recruitment of Dr. April Hartman, as division chief of General Pediatric and Adolescent Medicine. A graduate of Meharry Medical College who trained at MCG, Hartman quickly established herself back in Augusta as a great fit for the cohesive, comprehensive approach to family focused patient care and the education of future physicians that Hudson was working to strengthen. A true triple threat, Hartman also arrived as an advocate for the increasing number of patients with behavioral and developmental delays, and for fair treatment for all by spearheading diversity, equity and inclusion initiatives.
Hudson also established the Division of Pediatric Hospital Medicine, which a year later she expanded to include largely hospital-based infectious disease and pediatric palliative physicians. Pediatric hospital medicine was just designated as a board-certified specialty in 2016, a field which developed largely because of the changing dynamic in caring for kids. Like adult medicine, more care was being delivered to children on an outpatient basis and handled by general pediatricians. Outpatient care has changed too with an increasing number of pediatric outpatients needing care for the developmental and mental health problems that Hartman was helping spearhead at the Children’s Hospital of Georgia.
“The patients in the hospital now were in the ICU 20 or 30 years ago,” Hudson says. “Many of the patients who are in the ICU now did not live. The patients who were in the hospital 20 years ago are now being take care of as outpatients. It’s amazing the evolution of the complexity and the sickness.”
By last summer Developmental Pediatrician Jennifer Poon, MD, had joined up as chief of the Division of Developmental-Behavioral Pediatrics and as medical director of the new Center for Pediatric Development, Behavioral Health and Wellness. Poon had completed her fellowship in this increasingly sought-after subspecialty at the Medical University of South Carolina in Charleston and serves on the Executive Committee of the Section on Developmental and Behavioral Pediatrics of the American Academy of Pediatrics.
“There is an enormous need for behavioral and mental health services for children, which was there before COVID and was completely blown out of the water by COVID,” Hudson says, just a few weeks before a new Pew Research Center Report showed children’s mental health topped the list of parents’ concerns. Bullying was a close second.
“If you have a chronic illness then you are more prone to anxiety and depression. If you have anxiety and depression you are more prone to not taking care of yourself and doing your treatments and taking your medicine. So, you can’t treat one and ignore the other and expect to be successful,” says Hudson. She notes that at least a decade ago, the Cystic Fibrosis Foundation, a longtime leader in comprehensive and transformative care for complex illness, said Cystic Fibrosis Centers like the one at MCG had to have a mental health specialist as part of the care team. No doubt.
Her plans for the new comprehensive center were unfolding amid record reported levels of problems like ADHD, autism and depression among children and as the Academy of Pediatrics, American Academy of Child and Adolescent Psychiatry and the Children’s Hospital Association was declaring a national emergency in child and adolescent mental health. The 2023 Pew Research Center report was more of the unfortunate same.
The center got an incredible boost in 2022 by Kevin and Brittany Kisner of Aiken, South Carolina, with a $350,000 gift and a $5 million pledge to support essential groundwork. He is a professional golfer and she is a former speech language pathologist at the children’s hospital. An additional $4 million is actively being pursued to give the center a dedicated home in the children’s hospital, both to ease the process for children and families and further embrace collaboration between their caregivers. Hudson says the Kisners’ benevolent spirit enabled her to dream big, which she loves to do, on how to better address a clearly big and growing problem.
“I hope as we advance and gain more insight into this that we get better at prevention and that we can help children thrive and be well as opposed to just treating the illnesses that are already there,” Hudson says of the center which she insisted include wellness in its name.
On many other fronts, key recruits include Pediatric Geneticist Faizal Asumda, MD, who had just completed his clinical genetics and genomics residency at the Mayo Clinic in Rochester; Kristianna Singh, MBBS, who had finished her pediatric nephrology fellowship at Texas Children’s Hospital; and Pediatric Infectious Disease Physician, Ingrid Camelo, MD, who completed her fellowship at Boston Medical Center and is the new medical director of the CHOG Antibiotic Stewardship, Epidemiology and Infection Prevention.
All told in her handful of years as boss, Hudson has grown the Department of Pediatrics by 53 faculty members, with retirements and resignations accounting for just a handful of the spots, and eight more faculty starting this summer. She also has filled important blanks in areas like genetics.
The growth is hardly random, rather based again on the needs of children and math. Not unlike her commitment to the wellness of children, Hudson wants the same for the physicians — and everyone — who help take care of them. That means setting boundaries for how long physicians work when historically, mostly there have been no boundaries.
“That dehumanizes physicians in many ways because you are expecting us to be super humans and we are not,” she says. That means working 2,200 hours per year, rather than 24-7 365, is a reasonable expectation.
Boundaries have the additional benefit of enabling Hudson to give precise numbers to medical school and hospital administrators making the calls about who gets hired. “If you want a PICU that is open 24-7, 365 with a faculty member in house, this is how many doctors I need,” she says. A little cold, hard math also should help with faculty retention and provide objective data about what is needed for more growth.
Hudson does not care for boundaries, when it comes to meeting the needs of children where they are. Thirty booming pediatric outpatient practices are helping keep as many children as possible out of the hospital.
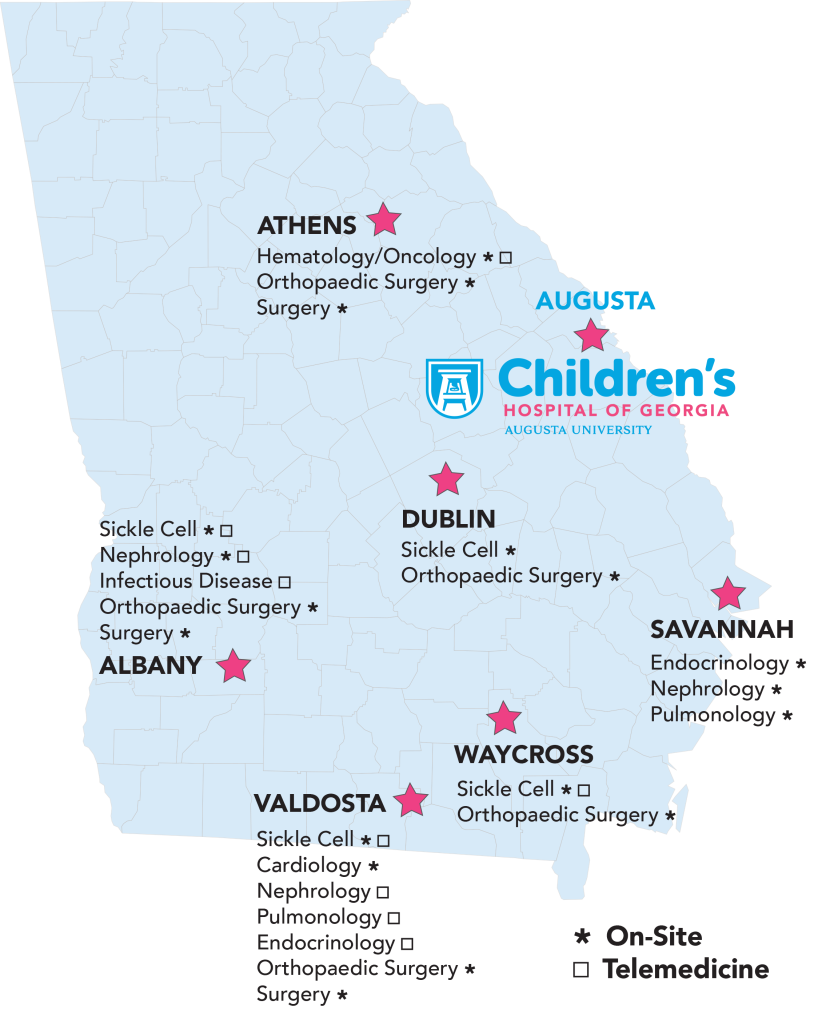
Outreach clinics in subspecialties like pediatric endocrinology, pediatric orthopaedic surgery and pediatric sickle cell, currently pepper the state. Like everything else, Hudson is looking at ways to grow the sites and enhance their efficiency and effectiveness for patients and physicians alike.
“We refer to it as windshield time,” Hudson says of hours spent traveling the expansive state to Savannah or Albany or Waycross.
Back to the math, physicians can’t see patients when they are seeing their windshields but it’s a great service to children and families and communities. In fact, Hudson counts some of those outreach clinic visits with patients among her favorite clinical encounters.
She is doing her usual talking with her colleagues and thinking about how to enhance access with also expanding programs in telehealth and telemedicine knowing that sometimes there is no replacement for face-to-face care.
And, keeping her battery charged.
Coda
Valera Hudson was 16, the only sister of three brothers when her youngest sibling, Richard, was hit by a car and killed. While she does not believe the tragic loss of her 8-and-a-half-year-old brother inspired her ultimate interest in pediatrics, she knows it inspired her ability to connect with people, to care about people and to walk beside families who also were losing children.
She has taken a lot of those walks. Caring for children with cystic fibrosis is a mainstay in pediatric pulmonology, and even before her fellowship, Hudson worked a lot with these patients in the year after her pediatric residency, a year Pediatric Chair Al Pruitt arranged for her, before she figured out what next.
During that time, the mother of her patient Dwayne McCutcheon asked why she would consider anything else when more doctors were needed to care for children like her son. Dwayne passed later that year, but his mother would send Hudson a Christmas card for the next 20 years.
“We didn’t have effective treatments for cystic fibrosis back then and we lost a number of amazing children, and somehow I was able to come along beside families and walk that journey with them,” she says.
“The children that I had the privilege of caring for, many of them were accepting and had a peace long before their parents. To watch these children fight to give their parents more time was the tension I was living in.” But the children also helped her. Fortunately, today 90% of these children are eligible for a drug that targets their specific, disease-causing gene mutation, treatment that has helped transform cystic fibrosis more often into a chronic disease children grow old with.
In fact, years ago, MCG and its health system expanded the Cystic Fibrosis Center to include an adult program in response to dramatic shifts in the survival rates of patients.
It goes back to softening the paradox.

“We do still have bad outcomes, but the majority of children are resilient and part of the joy of being a pediatrician is that kids can be really, really sick and recover and their resilience and their drive to live is just (she hesitates), it is something to behold.
Although she considers every patient at the children’s hospital her own, Hudson stopped directly taking care of patients midway through 2022, following the recruitment of Sunil Kapoor, MD, from Inova Fairfax Hospital for Children in Virginia, as the new chief of the Division of Pediatric Pulmonology. Kapoor joined the faculty in the last quarter of 2021 and Hudson wanted him free to make the division his own.
Every dollar counts
It was 1897, when a 10-year-old child befriended another child who was hospitalized in an adult ward of Augusta’s old City Hospital, MCG’s first hospital, because there was no other place for her.
In honor of her new friend, the child gave $1.20 to the Hospital Association, a communitywide initiative underway to build a new general hospital. The heartfelt gift of a child became the impetus for the association’s Children’s Ward Fund, and eventually the establishment of the Children’s Hospital Association to support construction of a freestanding children’s hospital as well.
Mary G. Cumming, whose family had helped develop the Augusta Canal and the city’s historic Summerville Neighborhood, helped lead the Children’s Hospital Association.
A few years later, New Yorker Grace Shaw Duff, who had spent winters in Augusta with her husband, wanted to do something to honor the community and the care her husband had received here. He had died, and a nurse who helped care for him in Augusta knew about plans for the children’s hospital.
Mrs. Cumming and the widow Duff met, and Mrs. Duff would give $25,000 to build the hospital and fully equip the operating room. The Wilhenford Children’s Hospital opened in 1910. The name, Wilhenford, combines the names of Mrs. Duff’s late husband William, her father Henry and her son Bradford.
Decades later, the Children’s Medical Center would first occupy the eighth floor of MCG’s adult hospital and opened as a freestanding hospital in 1998. The hospital was renamed Children’s Hospital of Georgia in 2013.
The new general hospital in Augusta would open in 1915 as University Hospital (now Piedmont Augusta), because of its affiliation at the time as MCG’s teaching hospital. MCG opened its own hospital in 1956.
If you would like to support the Children’s Hospital of Georgia and the MCG Department of Pediatrics please visit https://www.augusta.edu/giving/childrens.php, email philanthropy@augusta.edu or call 706-721-4001.