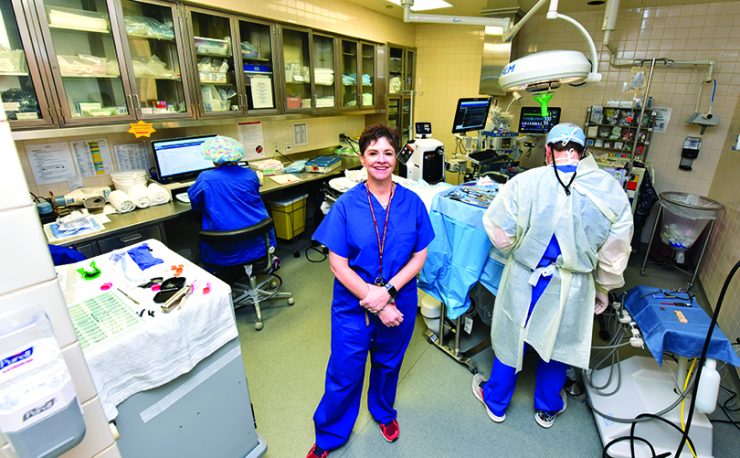
Pediatric Dentistry Department Works Closely With AU Health
Imagine your child sustaining extensive facial damage in a car accident . . . or receiving a cancer diagnosis . . . or having an oral infection with systemic complications.
As daunting as all these scenarios are, imagine the extra burden of having to ricochet between physicians and dentists to cover all the bases regarding treatment.
The Dental College of Georgia goes to great lengths to minimize this burden for its patients and their caregivers.
The DCG Department of Pediatric Dentistry has a highly collaborative and dynamic relationship with AU Health including the Children’s Hospital of Georgia (CHOG), AU Emergency and Express Care and AU clinics. The department also works closely with other DCG specialists, all housed under the same roof, to ensure its patients will be treated as effectively, expeditiously and conveniently as possible.
“Many of our patients travel long distances here for treatment,” says Dr. Tara Schafer, chair of the department, noting that the last thing their harried parents need is to navigate the coordination of multiple treatment sites.
DCG patients can leave the logistics to the health care team, Schafer said, thanks to the close working relationship of a multidisciplinary group of clinicians.
“We have seamless interactions with AU Health physicians, including referrals going both ways,” says Schafer. “We’re also on call 24 hours a day to handle patients in the emergency room who need dental treatment.”
This is vitally important for CHOG patients, she notes, who are particularly vulnerable, both physically and emotionally. A child whose mouth has been injured in an automobile accident, for instance, needn’t experience the added burden of being moved from site to site once they’ve arrived at the emergency room.
DCG students’ immersion in this collaborative environment begins immediately, Schafer says, with both dental and medical residents having the opportunity to complete clinical rotations in the neighboring facilities. The Department of Pediatric Dentistry offers a two-year residency program, choosing three to four dentists a year for admission. The residents treat patients in a variety of settings, including the CHOG operating room. All DCG pediatric dentistry residents also must complete MCG anesthesiology and pediatrics rotations. The rotations are invariably enlightening, Schafer says. For instance, MCG residents completing a clinical rotation in the dental school grow in their understanding of the potential systemic implications of even the most common oral conditions. “A lot of times,” she says, “medical residents don’t have much training in understanding how, for instance, a mouth full of cavities can affect overall health until they complete our rotation.”
Schafer notes that the faculty in both colleges fully embrace the added benefits for patients, students, residents and the community-at-large. “We have a great relationship with AU Health,” Schafer says. “The physicians send a lot of patients to us for dental treatment; for instance, we evaluate pediatric cancer patients before treatment, no matter what type of cancer they have, to ensure they don’t have abscesses or infections that will compromise their health when chemotherapy begins. Our staff also has block time in the operating room, treating patients who need to be sedated. And of course, with every dental specialty housed in the DCG, it’s very easy to consult with each other and work together.”
Telemedicine, which uses electronic information and telecommunication technology to enable long-distance communication with patients and health care providers, is yet another tool to consolidate expertise. The technology provides real-time specialized expertise to patients in rural, underserved communities, enabling DCG clinicians to help children from often-considerable distances.
Caregivers, Schafer notes, are extremely grateful. “Be it trauma or disease, a health problem for a child is very emotional for parents,” Schafer says. “It’s a difficult time. We do everything we can to make it as easy as possible for the family.”
This is exactly the mindset that drew Schafer, a DCG alumna, to pediatric dentistry. “I started dental school thinking I would go into orthodontics, but the first time I experienced pediatric dentistry, it just felt like home,” she says. “I was lucky enough to have great mentors, including (now-semi-retired Associate Dean and Professor in the Department of Pediatrics) Carole Hanes. I thought, ‘I want to be just like her.”
After earning her dental degree, Schafer completed a master’s degree in oral biology and an Advanced Education in Pediatric Dentistry program , then joined the faculty in 1996.
She has raised three children throughout her career, which she thinks adds an extra dimension of perspective. “I assure parents that everything I do for their child is exactly what I would do for my own,” she says.
She also considers every facet of the child’s well-being when developing a treatment plan. “There are always emotional components to treatment, and often social components as well. For instance, children whose teeth are knocked out in a car accident need to feel comfortable going back to school. We want to address both their short-term and long-term needs. We also treat a lot of special-needs patients, such as those with autism or Down syndrome, and we have a lot of techniques to make them as comfortable as possible, both physically and emotionally.”
The rewards, Schafer says, are tremendous. “We follow our patients throughout their childhood, and I’ve been here long enough to now be treating those children’s children.”
The bonds they form, she says, greatly ease what Schafer considers one of her most important tasks: patient and parent education. “Since dental caries are so preventable, we spend a lot of time on things like diet and oral hygiene,” she says. “We can usually fix everything, but we want to make sure we don’t see the same problems over and over again. We need parent buy-in. If we don’t address what got us here in the first place, we’re not making much headway. Parents need to be good role models; children need to see them taking care of their own teeth.”
Schafer also counsels parents to be cognizant of developmental limitations. For instance, “until children are in second or third grade, they don’t necessarily have the manual dexterity to clean their own teeth,” she says. “They’re unlikely to do it thoroughly or well,” so Mom or Dad should brush the child’s teeth — or at least oversee the process — until the child is around age 8.
These kinds of specific real-world tips can make a world of difference. But empathy and pragmatism are vital as well, Schafer stresses. “We have to acknowledge that even though parents will sometimes know the right thing to do, we don’t live in an ideal world. Cheap food, for instance, isn’t necessarily good for your teeth, and that may be the only kind some families can afford. We have to meet parents where they are.”
Schafer is also attuned to social or environmental issues that can affect a child’s oral health. For instance, tongue piercings, rare a generation ago but commonplace now, can pose infection risks. Oral problems related to eating disorders, including anorexia and bulimia, are on the rise among both girls and boys. “New issues are always coming into play,” Schafer says. “We make sure our students feel prepared to recognize signs and symptoms of issues like these and are comfortable addressing them with parents. We also have the resources necessary to quickly consult with the child’s pediatrician or a specialist and say, for instance, ‘I’m concerned about a possible eating disorder.’”
Schafer, whose department recently recruited a fourth full-time faculty member, feels incredibly fortunate to work for an institution that not only welcomes such interaction, but does everything possible to optimize it.
“This level of collaboration is definitely unique to the DCG,” she says. “I’m thankful every day for my career. I wouldn’t change a thing about it.”