At its core, an algorithm is a problem solver.
It can be a recipe for better brownies, help find the most direct route from point A to point B and potentially enable better outcomes from epilepsy surgery.
At his core, Dr. Fernando L. Vale too is an algorithm.
Vale grew up swimming, snorkeling and scuba diving in the clear waters of the Caribbean that surround the rectangular-shaped island of Puerto Rico. The family home was in Guaynabo, a coastal municipality in the San Juan metro area, but their heart was in the family farm in central, more rural Naranjito. His dad’s occupation was agronomy, working with dairy farms and looking after the quality of milk on the island, but the family farm is where you would most often find José Luis Vale. “When I was a little one, I used to go every weekend to that farm with him,” says Vale. There were cows, turkeys, rabbits, chickens always, and goats. There were mangos, potato-like yucca and plantains.
“It was a simple life,” he says, and they enjoyed the fruits of their labor. Vale fondly remembers his dad cooking and eating what they called Mofongo, fresh mashed plantains in a chicken broth, with barbecue chicken and tostones (fried plantains) piled alongside every Sunday. His mom Dalila’s mix of rice, chorizos (Spanish pork sausage) and gandules (pigeon peas) was Vale’s personal favorite.
There was always music and celebration. “We are happy people,” he says. Early life was good, and laid a foundation for family, farms, commitment and clarity of purpose.
The ultimate frontier
A neuroscience book he read in high school first laid out the brain as Vale’s “ultimate frontier” and made him want to be a doctor. “We know little, that is why I say ‘the ultimate frontier,” the chair of the Department of Neurosurgery at the Medical College of Georgia says of “this massive, super computer that we know little of.” In college at the University of Puerto Rico in San Juan, Vale took neurophysiology and neuroanatomy, which sealed the brain deal.
He did his undergraduate work in science at the University of Puerto Rico then went directly to the university’s medical school. Vale completed his neurosurgery residency at the University of Alabama Hospitals-Birmingham followed by a special Congress of Neurological Surgeons traveling fellowship in epilepsy and functional neurosurgery at Yale University and Washington University. He was recruited to the Department of Neurosurgery and Brain Repair at the University of South Florida Morsani College of Medicine right after in 1997.
In Tampa, he became director of the neurosurgery residency program in 2004, vice chair of the department in 2008, director of the Neuroscience Interdisciplinary Program in 2012 and director of the Functional and Epilepsy Division in 2014. He would double the faculty to more than 20 today. The residency went from one to two residents per year. He was neurosurgery tract director and medical student advisor. He started the epilepsy and functional neurosurgery fellowship. He helped expand to two new hospital systems, including negotiating contracts and neurosurgeons for affiliated hospitals. He was elected chief of the Department of Neurosurgery at Tampa General Hospital, a large teaching hospital that serves west Florida with a partnership of academic and private practice brain surgeons. He spoke and published about many aspects of neurosurgery, primarily his “passion” epilepsy.
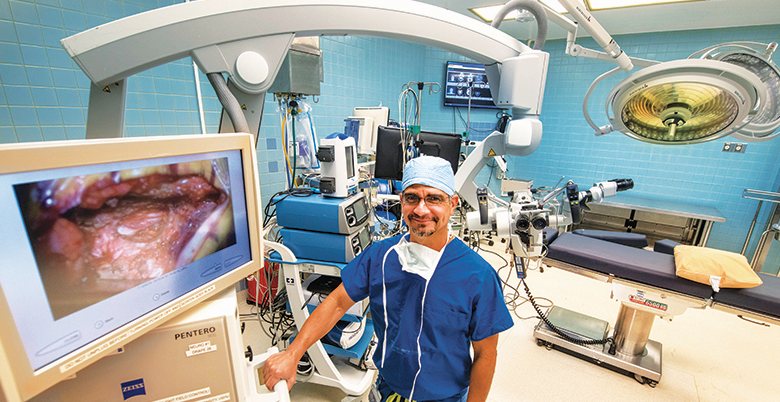
He met Elliot G. Neal. Vale calls the operating room his happy place, and that’s where he first met Neal, who today is a graduate of Morsani College of Medicine and a first-year neurosurgery resident in the program Vale helped build. “He complements my knowledge,” Vale says of the former field engineer who came to the operating room to provide technology support as an additional precision guide for Vale’s surgical tools. Like those moments in high school and college for Vale, Neal developed a passion for neuroscience and neurosurgery that drove him to quit an already successful career. “He is going to be a great surgeon one day. He has the passion.” Vale has told him that done right, the algorithm they are developing will hopefully help seal his success.
A short circuit
Epilepsy is excessive electrical activity that can throw an individual to the ground, eat away at their IQ and memories, even cause sudden death.
“Our brain at the fundamental level is an electrical system,” says Vale, and at the fundamental level a seizure is a short circuit. “The brain does not like it,” he adds pragmatically.
Seizures can happen to anyone at any time, often for no obvious reason, and become a vicious cycle of seizures, which damage the brain, which leads to more seizures and more damage.
While most often, the root cause of seizures is not known, the focal point in the brain from which the excessive electrical activity emanates sometimes can be found through an extensive neurological examination, with EEGs that map out the brain’s electrical activity and sophisticated imaging that lays out brain structure to see if there is an anatomic correlation.
“You can have a structural abnormality (like a tumor, scar tissue or bleeding) that causes electrical instability that can lead to seizure activity. You can have a connection problem, where we don’t see a structural abnormality, but which can still lead to seizures and epilepsy,” Vale says.
Either way, there is a connection problem that will surface as a spike and wave on an EEG and rock the brain. “The technology is not advanced enough that we can look at the microscopic level and know where the problem is,” he says. So when the MRI appears normal, doctors will add other noninvasive assessments, like a PET scan, to look for areas of hypometabolism in the brain when a seizure isn’t happening.
“It’s only when the seizure happens that there is increased blood flow, increased metabolism, because the brain is working harder, it’s spiking,” he says, mimicking the rapid “tuh, tuh, tuh” sound. Otherwise, a brain with epilepsy is less active.
Although he loves to run, Vale understands that we are still walking when it comes to epilepsy. He and Neal hope to pick up the pace.
Even though the list of pharmaceutical options now number more than 20, 20-30% of patients cannot get their seizures under control with medication. When it can be identified, surgery to eliminate the focus, or starting point, of a seizure is something surgeons like Vale specialize in, but that also is no guarantee.
Only about 66% of patients with the most common focal epilepsy, temporal lobe epilepsy, for example, are seizure free after the focal point is removed. “I would say that long-term cure maybe we are running around 65%, 70% at best, depending on the etiology,” he says. If there is a physical abnormality that correlates, like a scar, it tends to push up the percentage. But more often there is no clear anatomic abnormality and seizure free outcomes can drop closer to 50-50.
The algorithm
Neal and Vale’s algorithm adds physics and engineering to this mix of test findings to try to further define the network that explains the “epileptogenic” connection that may stretch across the length of the brain. Vale compares that pathway to a highway that has to be completely shutdown, otherwise the seizures may find a new starting point after he removes the old one. “What we are trying to understand is how all these connections work together to create epilepsy,” Vale says.
Bottom lines, they want their algorithm to help them and others better identify patients who will benefit from surgery, better identify which surgery they will most benefit from and likely results. Otherwise, surgery could do more harm than good. “You cut out a piece of the brain and it’s gone,” he says.
At the moment, the two are continuing to publish their findings and using the standard evaluation approach, both at MCG and in Tampa. But they are using the algorithm in tandem to test its efficacy, which means following patients for years to see if the ones they thought would most benefit do. The not-too-distant goal is a multicenter collaboration with MCG and AU Health System as the principal site.
“Epilepsy is my passion,” Vale says, the algorithm “his baby,” and the goal is a cure.
Time to grow
One of the things he tells his students is that time — and we — are finite, and a few years back, he came to the difficult realization that his time in Tampa was done.
“It was time to grow,” he says. He wanted to do more, be more, mentor more. “It was time for me to make something of my own, which I know I can do.” His tone is confident, but never arrogant. He simply had been a good lieutenant long enough and was ready to be the boss.
Late in the Spring of 2018, he applied for the job of neurosurgery chair at MCG. His first visit to MCG was in 1991 as a last minute interview for a residency slot. MCG was a definite “name” in epilepsy then as one of the first half-dozen Epilepsy Centers established in the nation. The renowned Dr. Herman F. Flanigin started the Epilepsy Surgery Program component that would enable the Augusta-based program to become an accredited, top Level 4 Epilepsy Center. Flanigin had studied at the Montreal Neurological Institute and, along with institute Director Dr. Wilder Penfield, authored the first paper outlining the use of temporal lobectomy to treat epilepsy. Flanigin led the surgery program he started for more than a decade. Dr. Joseph Smith, who came to MCG to study with Flanigin in 1985, led next. Vale met Smith the day of his residency interview, and when he started his chair’s job at MCG in February 2019, one of his first plans was to reconnect with Smith, who he learned had died just weeks before.
At MCG, Vale is rebuilding a team of neurosurgeons that had dwindled in recent times to just a handful. Dr. Martin Rutkowski, an expert in surgical neuro-oncology and skull base surgery, was one of his first recruits, fresh out of his neurosurgery residency at the University of California, San Francisco, and an open and endoscopic skull base surgery fellowship at the University of Southern California. Dr. Todd Maugans, pediatric neurosurgeon who had served as chief of the Division of Pediatric Neurosurgery at Nemours Children’s Hospital in Orlando and chair of neurosurgery education at the University of Central Florida, is another. Spine Neurosurgeon Dr. Michel Pare, a native of Montreal who did his fellowship training at the Mayo Clinic and practiced in first Dalton then Albany, Georgia for the last 22 years, is another.
As October was closing, there was an offer out to a second functional neurosurgeon and there are plans for adding depth in other areas including pediatric neurosurgery, spinal neurosurgery and malignant and benign tumor surgery. Vale also has hired a second basic scientist, Dr. Kumar Vaibhav, whose focus includes improving repair of a traumatic brain injury and who was mentored by longtime faculty member, neuroscientist Dr. Kris Dhandapani.
Vale worked collaboratively with the Georgia Cancer Center and Department of Neurology to recruit Dr. John W. Henson IV, medical director of the Ivy Center for Advanced Brain Tumor Treatment and director of the Swedish Neurofibromatosis Center at the Swedish Neuroscience Institute in Seattle. Henson has also has served as chief of Oncology Services at Piedmont Healthcare, Inc., in Atlanta and on the faculty of Harvard Medical School. Vale notes that he has found the Department of Neurology, under the leadership of Dr. Jeffrey Switzer, exceptional, essential partners in what he is now trying to build in their surgery counterpart. The two departments have already started a neuroendovascular fellowship in July 2019 under the direction of 2002 MCG graduate Dr. Scott Y. Rahimi (MCG Medicine, Spring/Summer 2018).
Vale has definite plans for restoring the epilepsy and functional neurosurgery fellowship as well. Long-time epileptologists in the neurology department, Drs. Anthony Murro and Yong Park, who specialize in adults and children, respectively, and newer-comers MCG graduates Drs. Debra Moore-Hill (see page 51) and Suzanne Strickland also are now his practice partners.
“We have the building blocks. Now we are putting the building together,” he says, noting that optimizing clinical care and access to it are important first pieces so that the more academic aspects, like a larger residency program and the planned new fellowship, as well as clinical research can happen. So is ensuring a well-rounded neurosurgery program that meets the subspecialty needs of the community.

Back to the farm
Like his earliest days, Fernando Vale’s life is good, and the professional choices he has made still inspire and mostly keep a smile on his face.
“I wanted to be a neurosurgeon because it was special, unique, challenging. But then when you actually start dealing with neurosurgery, you realize this is really a privilege that you can work in somebody’s brain. That is so special,” says Vale.
Epilepsy and functional neurosurgeons are considered the most “cerebral” of the brain surgeon types, Vale says, which can play out badly when the obvious associated stress is expressed badly. Vale by contrast seems calm, happy, reasoned. He keeps his stress down with his running “just me and the wind” and gardening, which takes him back to the farm and home.
“Remember, it all comes from the land,” says Vale whose daughter, Neuro ICU nurse Gabriela “Gaby” Cochran-Vale and her husband Brian Cochran live on and work the 30-acre farm in nearby Aiken, S.C., the family is now building in the Vale tradition. Vale and his wife Lynda live in Augusta’s historic residential district of Summerville, just up the hill from the medical school campus.
Like his parents, they make weekend sojourns to the farm, which is now the home of a small herd of goats, a menagerie of rescued dogs and cats, the latest addition is a rescued donkey, as well as an expansive garden, with tomatoes, all kinds of peppers, lettuce, cucumbers and pumpkins, where the brain surgeon likes getting his hands dirty.
Other highlights
Biological son Fernando R. Vale, a graduate of the U.S. Naval Academy, today is an intelligence officer who was just promoted to First Lieutenant in the U.S. Marine Corps. He and the Vale’s “adopted” son (in quotes because there was never an official adoption) Thomas Cadwell were best friends in high school, both in junior ROTC, then the younger Vale went to the Naval Academy and Cadwell went into the Air Force. Long, important story short, life with his biological family has been distant, but life with the Vales has been close. Cadwell, is now a nursing student at Augusta University College of Nursing also living on the farm. “We are his closest family,”
says Vale.
Vale loves teaching and mentoring, which he says are key to the algorithm of a better future for both student and educator. “It keeps you young. It’s a constant challenge. I want our students to be better than me one day, all of them. That is the cycle of life.”
In a do-over, Vale says he would have at least an early collaborator to help him get where he wanted to be. As it was, he did not have a true mentor, rather thought he could make it on his own. He clearly did, but there were tradeoffs. “This is what I tell the guys here: ‘I will be the bad guy. I will pick up the fight. Tell me where you want to go, and I will help get you there.’” But they have to have the passion, the drive to get there, he also tells them.
He acknowledges that being a good boss is a tough job that a thick curriculum vitae cannot necessarily prepare you for. He prefers the straight talking, doing the work and caring about other people’s success approach of leaders like MCG Dean Dr. David Hess and Dr. Charlie Howell, pediatric surgeon and MCG graduate, who is now leading MCG’s physicians practice group.
Other Accomplishments
Vale’s areas of professional interest also include movement disorders, like Parkinson’s, which is also fundamentally about chemical imbalances and electrical and connection problems.
“The brain is like the government,” he says, “a bunch of checks and balances. When you lose a balance or you lose one corner, you get this unbalanced stimulation that can lead to too much movement or too little or can lead to dementia or behavioral problems. It all about checks and balances.”
He has served multiple times as a guest examiner for the American Board of Neurological Surgery and has been an examiner in functional and epilepsy surgery since 2017. He calls it a duty and pleasure that he hopes will help ensure the quality of his chosen profession.
He has been a member of the Executive Committee of the Southern Neurological Society since 2005, and has served as secretary and president.
Vale holds the Marshall Allen Distinguished Chair, which honors the late, longtime neurosurgery chief of nearly 30 years. Neurosurgery was made an academic department at MCG in 2002.
Note: The Epilepsy Center at MCG and AU Health remains a Level 4, among some 170 programs accredited as Level 3 or 4 by the National Association of Epilepsy Centers. Level 3 centers do not offer the more complex surgeries like the ones Vale performs.